Gallbladder Surgery Cost in Pune
BlogIf you’re considering gallbladder surgery, you may be wondering about the costs involved.
Fortunately, modern treatments like laparoscopic surgery have made this type of procedure relatively affordable for most patients.
Here at our clinic in Pune, we offer a range of options and costs to suit various budgets and preferences – from low cost packages to high-end solutions.
In this blog post, we’ll provide an overview of what you can expect when it comes to the cost of gall bladder surgery so that you can make an informed decision about your surgery needs.
Summary
Gallbladder surgery (cholecystectomy) is a safe and effective treatment for gallstones and related complications.
In Pune, laparoscopic gallbladder surgery is the most common option, with costs typically ranging from ₹30,000 to ₹60,000.
The final cost depends on several factors such as the type of procedure, hospital facilities, surgeon’s experience, and case complexity.
Additional expenses may include pre-operative tests, anesthesia, medications, hospital stay, and follow-up visits.
Most health insurance policies cover gallbladder surgery, and cashless treatment may be available with prior authorization.
Choosing an experienced surgeon, opting for package pricing, and timely surgery can help keep overall costs under control while ensuring safe care.
What is Gallbladder Surgery?
Gallbladder surgery is a procedure that removes the gallbladder, a small organ located behind the liver.
It is used to treat gallstones, which are collections of hardened bile that can cause pain and other digestive issues.
Gallbladder removal is also known as cholecystectomy and it’s generally a safe and effective treatment for treating gallstone-related problems.
How much does Gallbladder Surgery cost?

The cost of gallbladder surgery in Pune varies depending on the type of procedure you choose.
Laparoscopic or keyhole surgery is usually more affordable than open gallbladder removal, which requires a larger incision.
Most patients can expect to pay between ₹ 30,000-60,000 for laparoscopic cholecystectomy at our clinic in Pune, with the upper end being reserved for more complex cases.
Are There Any Other Costs Involved?
In addition to the fees for the procedure itself, there may be additional costs associated with preoperative tests like imaging and laboratory testing that are needed to confirm your diagnosis and ensure your safety during surgery.
These charges can range anywhere from ₹ 2,000-20,000 or more depending on the type of tests required.
9 important Factors that Decide the Cost of Gallbladder Surgery
1. Type of Procedure
Laparoscopic surgery is generally more affordable than open gallbladder removal, with the latter being reserved for more complex cases.
2. Clinic or Hospital
The fees charged by clinics and hospitals may vary depending on the location and reputation of the facility.
3. Experience of Surgeon
The experience level of your surgeon can have a significant impact on the cost, as experienced surgeons tend to charge higher fees than less experienced ones.
4. Preoperative Tests
These are important tests performed before your procedure to ensure your safety and confirm your diagnosis, and they can add up quickly.
5. Anesthesia Costs
If you require general anesthesia during surgery, there will be additional costs associated with this.
6. Hospital Stay
Depending on the complexity of your case, you may need to stay in hospital overnight or even longer – and this will come at an additional cost.
7. Medication Costs
You may require pain medications and other drugs after your procedure, which can add up quickly.
8. Follow-up Visits
Most patients require follow-up visits with their doctor for monitoring your recovery, and these also come at an additional cost.
9. Insurance Coverage
If you have health insurance, some or all of these expenses may be covered by your policy – so make sure to check with your provider beforehand to get a better understanding of what is covered and what isn’t.
Is Gallbladder Surgery Covered by Insurance?
Yes, gallbladder surgery is usually covered under most health insurance policies, especially when performed for symptomatic gallstones.
Depending on your policy:
Cashless surgery may be available
Pre-authorization may be required
Coverage may include surgery, hospital stay, and anesthesia
Our team can assist you with insurance documentation and help you understand your coverage before the procedure.
How to Minimize the Cost of Gallbladder Surgery?
While gallbladder surgery is a common and safe procedure, there are several practical steps you can take to keep the overall cost under control without compromising on safety or quality of care.
1. Choose Laparoscopic Surgery Whenever Possible
Laparoscopic gallbladder removal usually costs less in the long run due to a shorter hospital stay, faster recovery, and fewer post-operative medications compared to open surgery.
2. Opt for Package Pricing
Hospitals and clinics that offer all-inclusive packages often help reduce unexpected expenses. These packages typically cover surgery, anesthesia, hospital stay, and basic medications.
3. Use Health Insurance or Cashless Facility
If you have health insurance, check whether your policy covers gallbladder surgery. Cashless treatment can significantly reduce out-of-pocket expenses.
4. Complete Pre-Surgery Tests at One Center
Getting all required blood tests and imaging done at the same clinic or hospital can be more cost-effective than visiting multiple diagnostic centers.
5. Avoid Delaying Surgery
Postponing surgery can lead to complications such as infection or inflammation, which may increase treatment complexity and overall costs.
6. Choose a Short Hospital Stay When Medically Safe
Many patients can be discharged the same day or within 24 hours after laparoscopic surgery, helping reduce room and nursing charges.
7. Follow Post-Surgery Instructions Carefully
Proper diet, medication adherence, and timely follow-ups can prevent complications and avoid additional medical expenses.
By planning ahead and choosing the right surgical team and treatment plan, patients can significantly reduce the cost of gallbladder surgery while ensuring safe and effective care.
How to choose the best surgeon for your surgery?
To ensure you get the best possible outcome from your gallbladder surgery, it’s important to choose a qualified and experienced surgeon who is board-certified in their field.
Make sure to do some research on the doctor’s background, qualifications and experience before committing to a procedure.
At our clinic in Pune, we offer comprehensive packages that include consultation with an experienced surgeon and access to all necessary tests and treatments required for gallbladder removal at affordable prices.
Our team of surgeons are highly skilled and experienced, so you can rest assured that you’ll be receiving top-notch care throughout your treatment.
We hope this blog post has given you a better understanding of what you can expect when it comes to gallbladder surgery cost in Pune.
If you have any questions or concerns, feel free to contact us and we’ll be happy to help.


 +919011100010
+919011100010 




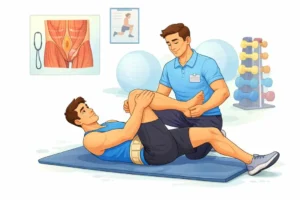 Physical therapy is another non-surgical treatment option that may be helpful for individuals with hernias.
Physical therapy is another non-surgical treatment option that may be helpful for individuals with hernias.